- Home
- Learn
- Healthcare
- Duplicate Patient Records: Causes, Costs and Fixes
HEALTHCARE
Duplicate Patient Records: Causes, Costs and Fixes
Contents
Duplicate patient records occur when the same patient is assigned multiple records within a single healthcare system. A report from the American Health Information Management Association shows that a typical hospital has a 10% duplication rate. The average rate of data duplication at large healthcare institutions hovers between 15-16%, which means there could be up to 120,000 duplicate records among every 1 million patient records.
The clinical consequences go far beyond just the balance sheet – duplicate records mean multiple incomplete records, which can lead to information mismatch and loss. In fact, a 2025 BMJ Group study links duplicate medical records to 5x heightened risk of inpatient death and 3x likelihood of ICU-level care needs. A majority of health systems in India and the USA still operate without a national unique patient identifier – and with organizations running multi-system intakes, duplicates are easy to create and hard to spot.
In this article, you will learn about what causes duplicate patient records, their impact,and solutions to streamline patient records.
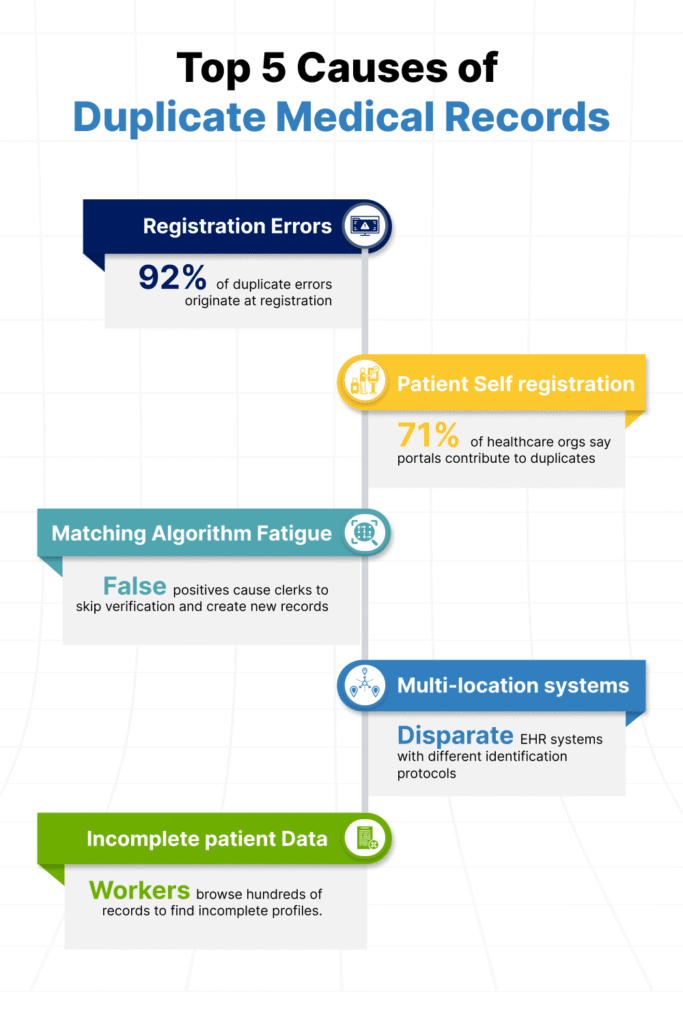
Duplicate medical records can be caused by the duplicate or partial entry of patient data, where a patient’s information is stored with slight variations in name spelling, phone number, insurance details or ID number. Most duplicates are created during the initial touchpoints: scheduling, registration, and inbound. And with digital health apps on the rise, patients might use different contact channels to find and book an appointment. Case in point: A 2022 study by Patient ID Now found that 71% of healthcare organizations agree that allowing patients to use self-serve/self-schedule portals, have led to an increase in duplicate patient records.
Misspellings, incorrect dates of birth or social security numbers, failure to verify core data elements, and improper matching algorithms are the main culprits of duplicate medical records. When matching algorithms are overly (or insufficiently) sensitive, the system flags too many false positives. This leads to the admission clerks becoming fatigued and simply creating a new record, rather than reviewing possible matches.
To catch possible duplicate records early-on, here are some patterns to watch out for:

Duplicate medical records have vast financial, clinical and operational impacts – from over $1 million in losses and 5x higher rates of patient fatality post-hospitalization to 30% higher rates of readmission and creating decisional distortion.
Every year, large healthcare facilities spend more than $1 million fixing duplicate data issues including staff time, technology costs and downstream operational expenses. Given that duplicate medical records increase the risk of worsening a patient’s outcome, lawsuits may follow – the annual malpractice cost caused due to duplication is $1.7 billion. A 2021 study of 1500 health technoloy managers found that around 35% of denied claims originate from inaccurate patient information – which arise from duplicate medical records.
Here are a few insights from the 2025 BMJ study. It’s a propensity-matched cohort analysis of 103,000 medical records across 12 U.S. hospitals, that evaluated the association between duplicate medical records and patient outcomes.
While this was an observational study (that identified associations rather than definite causation), a clear pattern is revealed: duplicate records create fragmented pictures, leading to incorrect or delayed care decisions.
Duplicate medical records can cause decision distortion, which arises from corrupt dashboards. When staff and leadership have no clear visibility of OPD-to-admission conversion, no-show rates, duration of stay, and other patient-centric metrics, “data problem” becomes an “operations problem”. Here’s how it affects different healthcare organizations:
Duplicate medical records disrupt healthcare operations by creating friction across departments. When teams across various departments (registration desk, care coordination team, finance team and compliance team) cannot work in sync, information is missed out – leading to creation of duplicate records.
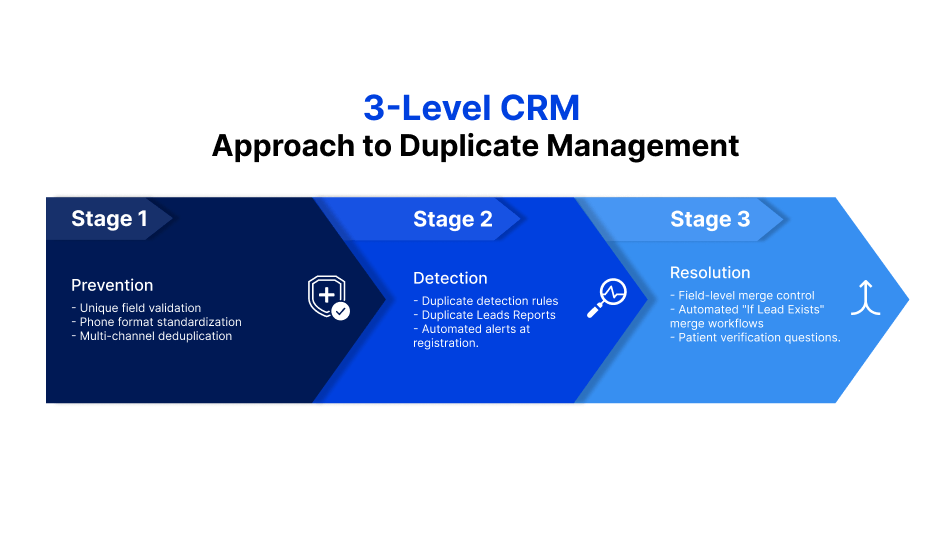
records: prevention with unique fields, detection with duplicate reports, and resolution with automated merging
Preventing the creation of duplicate medical records requires a framework strict enough to stop duplicates, but practical enough for busy teams. This can be created by defining a consistent set of fields across intake channels, standardizing front-desk staff operations and using a healthcare CRM to detect and automatically merge duplicate leads. By implementing the perfect combination of rules, behaviors and controls, technology can aid staff in ensuring reliable procedures are executed.
Here’s a framework that can help you prevent duplicate patient records:
Step 1: Define your “Minimum identity dataset”
– Use a consistent set of fields across every intake channel, such as first name, last name, DOB, primary phone number, locality, email, sex, and payer/TPA.
– In India, capture ABHA when available. With almost 80 crore ABHA accounts created to date, it can improve continuity across organizations when used consistently.
Step 2: Standardize a search-first workflow
Ensure that staff search for at least 2 attributes before creating a new record. Make this a standard and measurable SOP.
Step 3: Standardize inputs
Create an easy-to-follow format for phone numbers, name fields,and DOB inputs. These small controls prevent larger downstream errors.
Step 4: Design for privacy
India’s DPDP Act 2023 and USA’s HIPAA regulatory guides establishes frameworks for processing digital healthcare data. Capture only what you need, store it securely, and audit access controls regularly.
Now, it’s time to connect this framework to the system that manages your intake workflow: your healthcare CRM.
The most effective way to “clean up” duplicate records is to prevent them at the point of entry. Modern healthcare CRMs help prevent, detect, and provide a resolution at intake itself.
Here’s how:
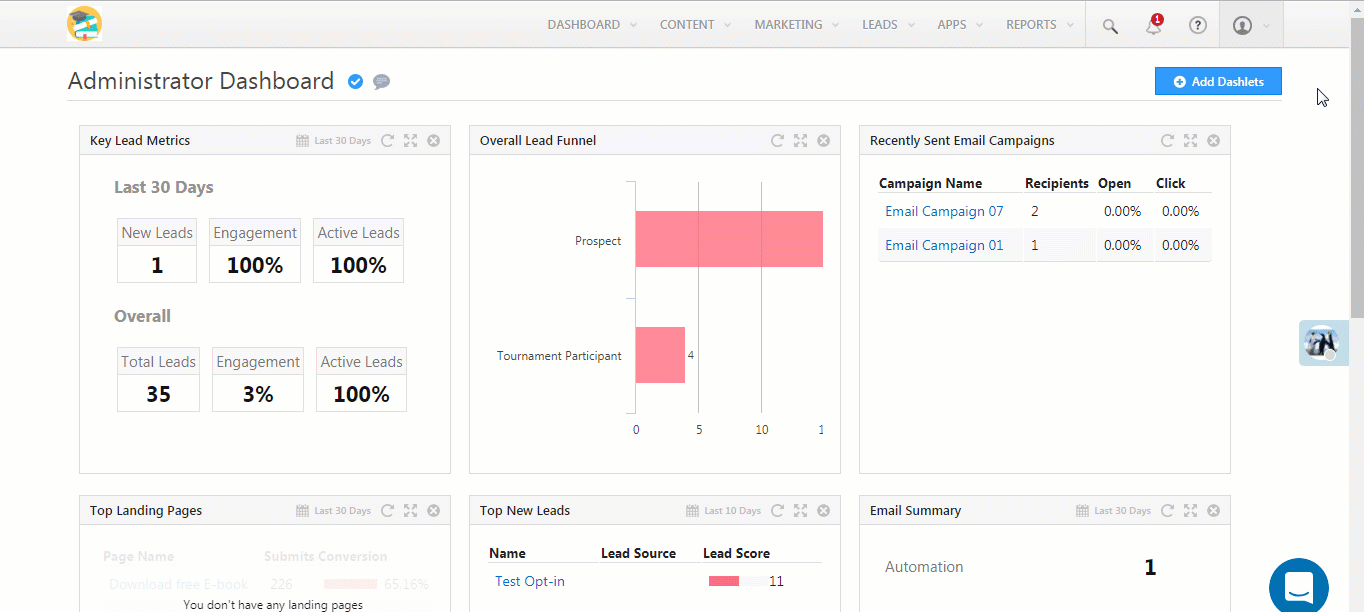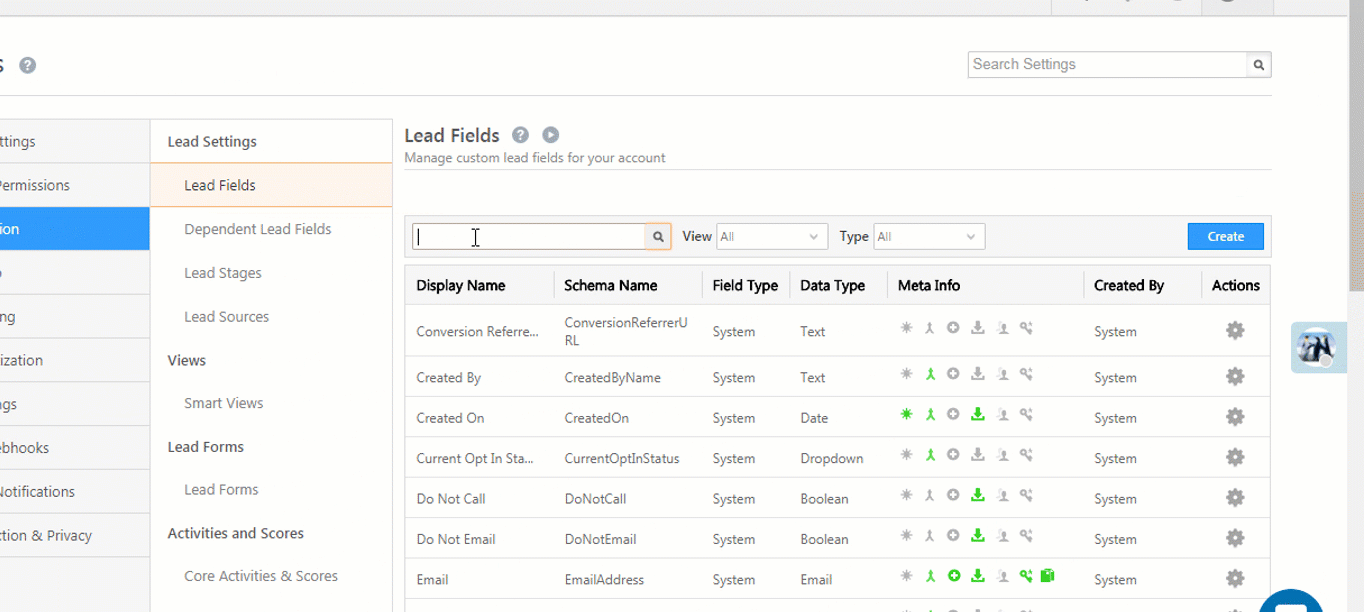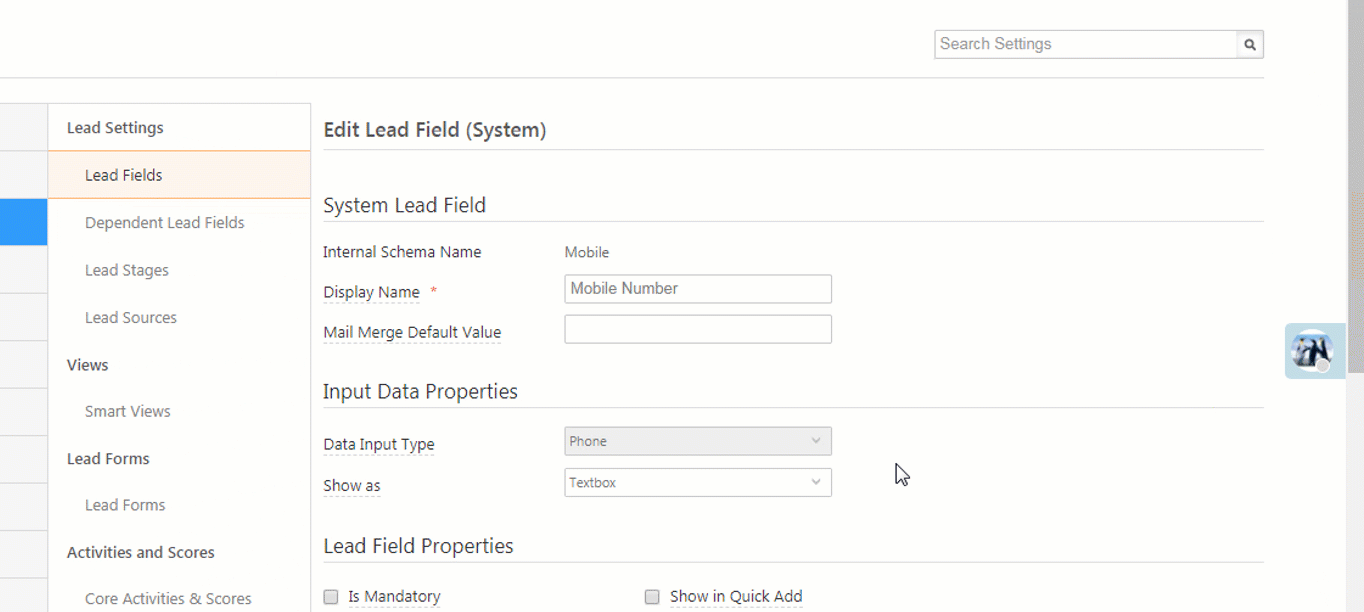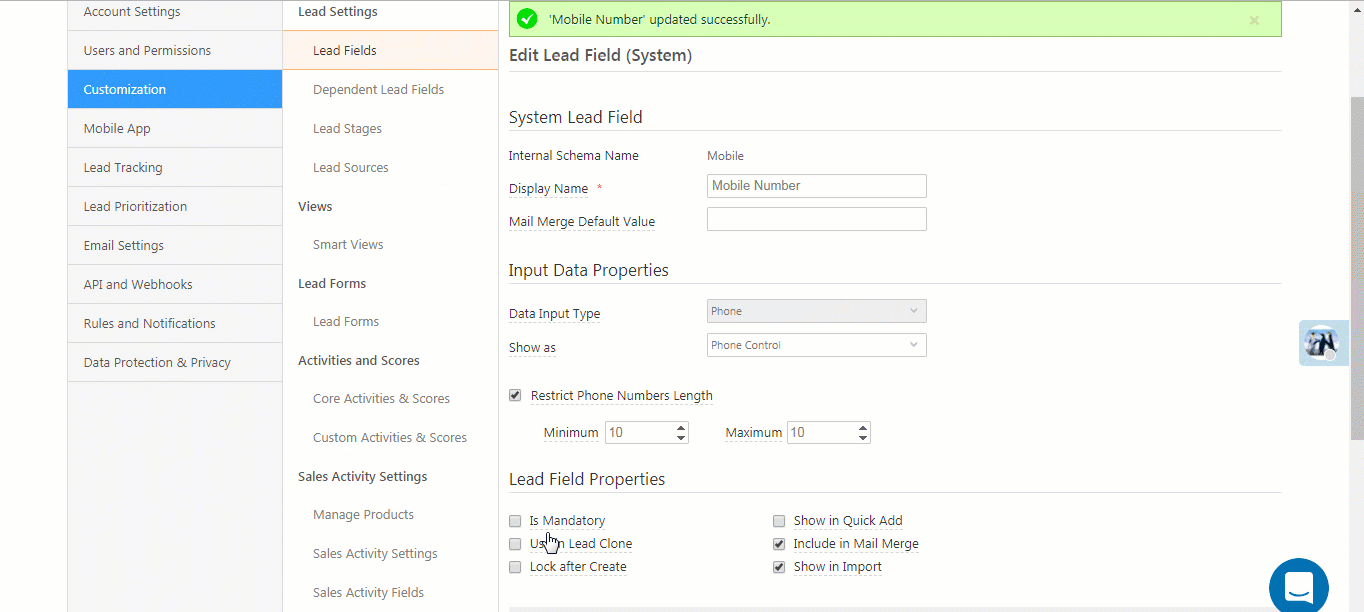
Overlays are caused when two different patient data are intermingled within one chart. You can merge duplicate medical records without creating overlays by triaging your records, capturing and segregating every unique identifier, and maintaining a continual hygiene check.
Step 1: Triage your records first
Start with high-confidence matches such as exact phone number, ABHA/MRN ID, Insurance ID. It’s best to do this in combinations – such as phone number + DOB, or Insurance ID+ABHA ID.
Step 2: Flag records that need a second review
If you feel like your match is ambiguous, flag the records you want your clinicians to cross-verify. They can then view both histories and pass the correct information to the data integrity team.
Step 3: Capture and preserve every identifier
During migrations or mergers, capture every available identifier (including legacy MRNs) and maintain their correct format. As we’ve seen, even small shifts can create new duplicates or overlays. You can always standardize these identifiers later.
Step 4: Close and standardize the loop
Once you’ve identified your duplicates and sorted them, implement a workflow that’ll keep a constant “check” intact – so your system can automatically capture, flag and correct duplicate records.
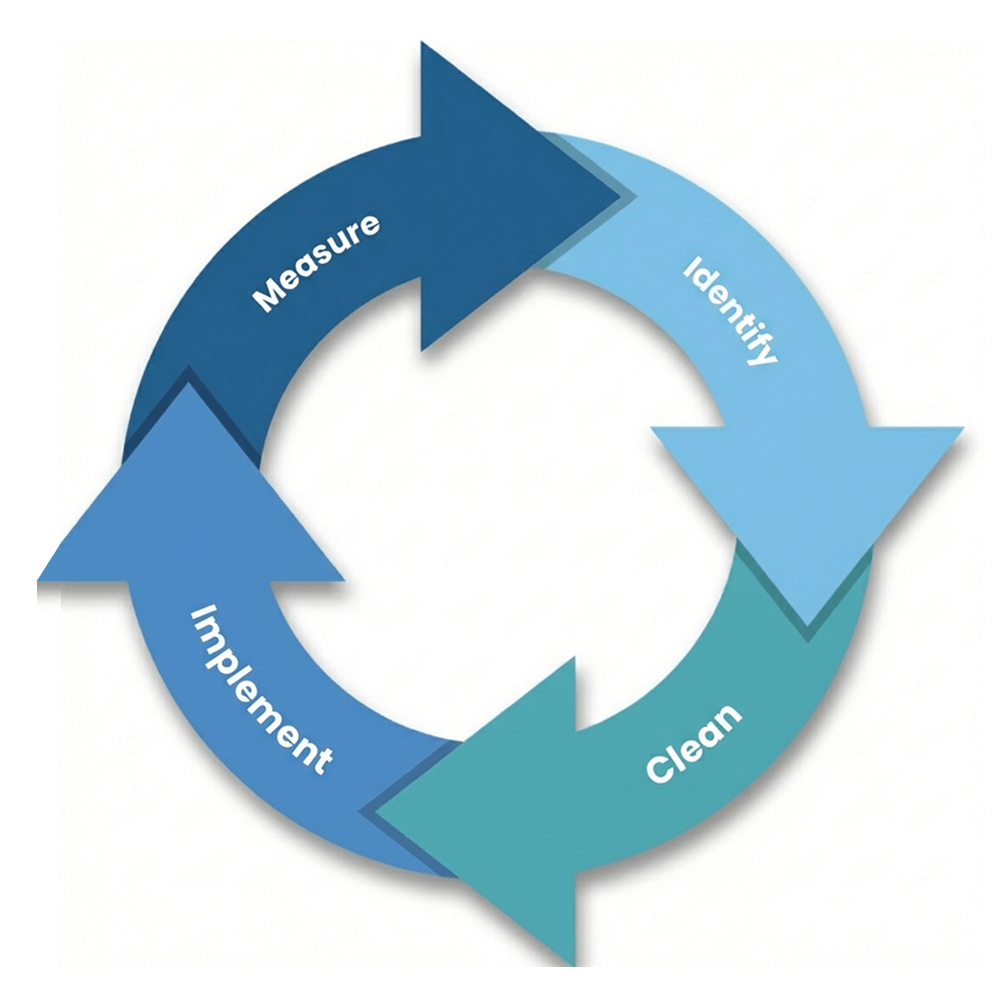
A duplicate patient record audit framework can help your organization stay compliant and avoid lawsuits to do malpractice. To build such a framework, follow these 4 essential steps: identify, clean, implement and measure. Here’s how you can come closer to achieving a 1% duplication rate, inspired by AHIMA’s ICMMR cycle:
1. Identify:
2. Clean:
3. Implement:
4. Measure:
The best teams treat duplicate records as “process defects” and eliminate the cause, not just the duplicate record!
Ready to eliminate duplicate records and strengthen your patient’s data integrity?
Ans; A duplicate record simply means a patient has more than 1 medical record number, in the same system. An overlay is when 2 different patient’s data mingled in one chart. An overlap is when the same patient has different identifiers across facilities, commonly occurring post-acquisitions.
Ans: By using a multi-step verification approach, ensuring registration and front-desk staff follow search-first SOPs and standardizing input formats, you can prevent duplicate patient records.
Ans: Looking into and cleaning up duplicate patient records should be a shared program across operations, data team and IT. Operations team can own adherence to protocols, data team can comb through data and IT team can own integrations and audit logs.
Ans: The safest way to merge duplicate medical records is to triage high-confidence matches first, flag uncertain reviews and preserve legacy identifiers during system mergers or changes.
Ans: A healthcare CRM helps prevent duplicate patient records by providing unique field identifiers, standardizing input formats and creating easy-to-follow workflows for registration staff.
Ans: Yes, merging duplicate patient records are compliant with data protection laws such as DPDPA and HIPAA acts – as long as the process maintains a completely traceable audit trail, preserves the integrity of previous data and follows organizational-level data governance policies.